Malaria: Uganda and Rwanda battle misinformation and lack of education in race to roll out vaccine
The vaccine is a significant step in eradicating a disease which has killed more than 409 000 in 2019, but vaccine hesitancy presents problems for the roll out in sub-Saharan Africa, writes Amanda Coakley
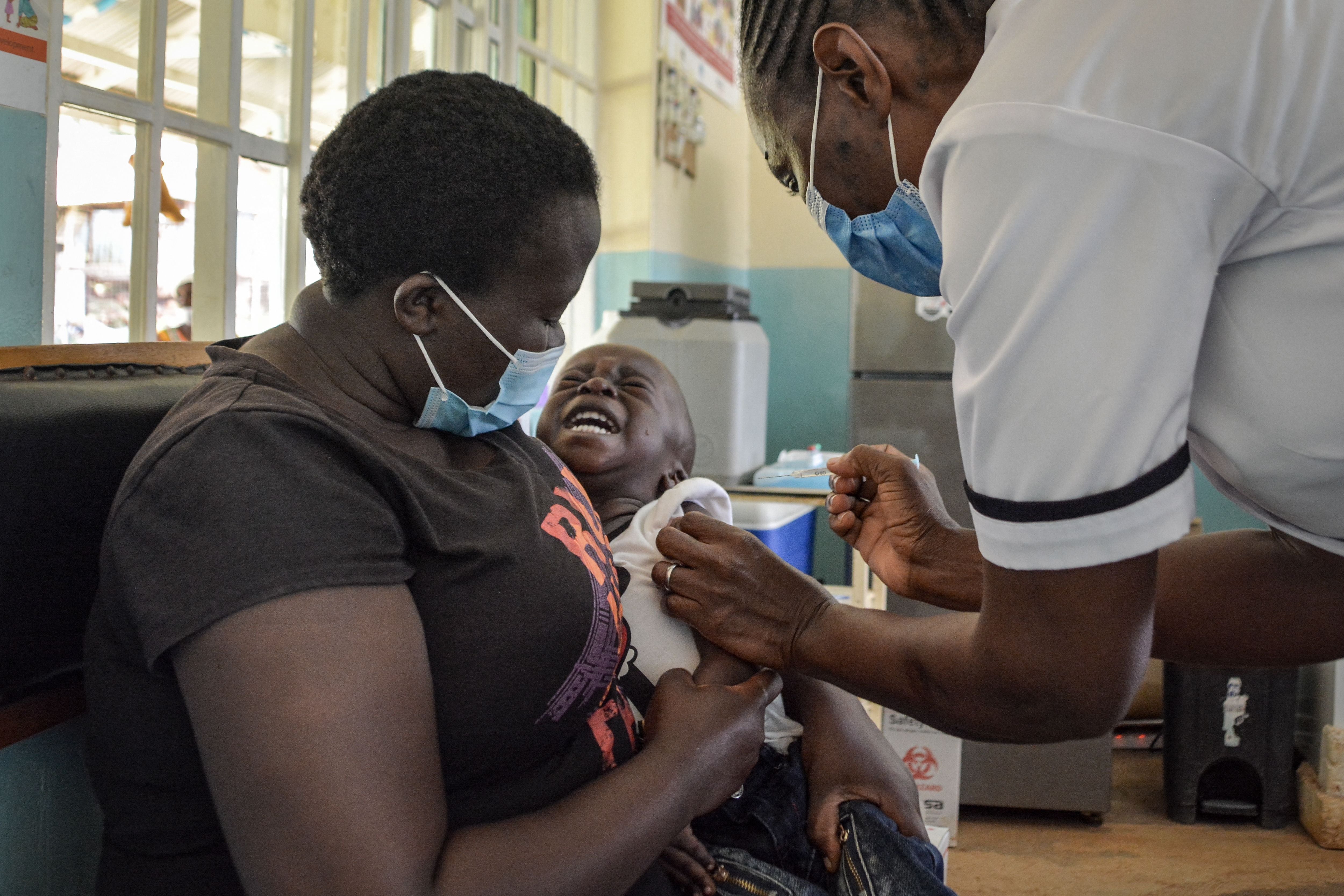
On Thursday Simon Loput’s two-year-old daughter Jane became ill with a fever. As soon as possible the young father and his wife rushed to a nearby hospital in Uganda’s northern Nabilatuk District where their worst fears were confirmed: Their toddler had malaria. Simon’s ability to react quickly had come from experience, the mosquito-borne disease has plagued his community for generations.
“My daughter is improving now but it’s still frightening. Our hospitals are not very comfortable as there is very little space in the wards,” he told The Independent via video call. “It’s also disturbing in terms of money because sometimes the medicines in the hospital are not enough, so I had to spend a lot to buy the drugs my daughter needs.”
The day before tragedy struck the Loput family, the World Health Organisation (WHO) approved the rollout of the world’s first malaria vaccine in sub-Saharan Africa and other areas with moderate to high levels of transmission. Known as RTS,S, or Mosquirix, the vaccine was developed by GlaxoSmithKline (GSK), a British pharmaceutical company headquartered in London. In development for over 30 years, the efficacy of RTS,S is low at 39% and only acts against P. falciparum – the most dangerous malaria parasite globally. Nonetheless it’s a significant step towards eradicating a disease that caused more than 409,000 deaths in 2019, the majority of which were children under five.
Subscribe to Independent Premium to bookmark this article
Want to bookmark your favourite articles and stories to read or reference later? Start your Independent Premium subscription today.
Join our commenting forum
Join thought-provoking conversations, follow other Independent readers and see their replies